Most practices don’t know they have a billing problem. They know they have a cash flow problem. They know claims are taking longer to pay. They know the front desk is always busy but the numbers don’t reflect it.
The billing looks like it’s working. The revenue doesn’t add up.
That gap — between activity and results — is where practices quietly lose tens of thousands of dollars every year.
Most practices don’t know they have a billing problem. They know they have a cash flow problem. They know claims are taking longer to pay. They know the front desk is always busy but the numbers don’t reflect it.
The billing looks like it’s working. The revenue doesn’t add up.
That gap — between activity and results — is where practices quietly lose tens of thousands of dollars every year.
What 190-Day AR Actually Means
When a client came to Dr. Billerz, their aged AR had stretched to 190 days. That number sounds like a payer issue. It rarely is.
190-day AR means a claim was submitted, something went wrong, and nobody caught it in time. Then it happened again. And again. Until the backlog was so deep that normal billing operations couldn’t absorb it.
Denials were recurring. Cash flow had become unpredictable — not because the practice wasn’t seeing patients, but because revenue wasn’t arriving on any reliable timeline. The front desk was spending hours chasing balances instead of managing the patient experience.
This isn’t a staffing failure. It’s a structural one. When your billing system is built to submit claims — not to own what happens after — the cracks compound over time.
The 30-Day Forensic Audit
Our first step wasn’t to work the backlog. It was to understand it.
We ran a 30-day forensic audit across the practice’s entire revenue cycle. That means claim-by-claim diagnosis: where did this denial originate? Is this a coding error, an eligibility gap, or a payer-specific pattern that keeps recurring? What’s the actual root cause — not just the symptom?
What we found was consistent with what we find in almost every new client: the problems weren’t random. They were systemic. The same errors were generating the same denials, over and over, because nobody had traced them back to their source.
Coding mismatches. Eligibility verification gaps. Insurance payer issues that required a different submission approach. Each one fixable — but only once identified.
What Changed
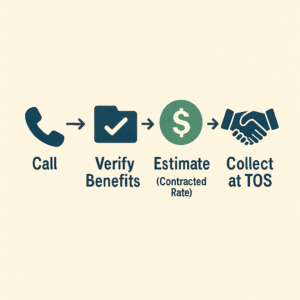
Once the root causes were mapped, we moved from reactive to controlled. Claims weren’t just submitted — they were scrubbed, verified, and tracked. Denials weren’t logged and queued — they were remediated at first touch. Aging AR wasn’t monitored — it was worked down systematically.
This is the difference between a billing team that processes claims and a revenue control system.
The Results
90 days after the audit began, the numbers told a different story.
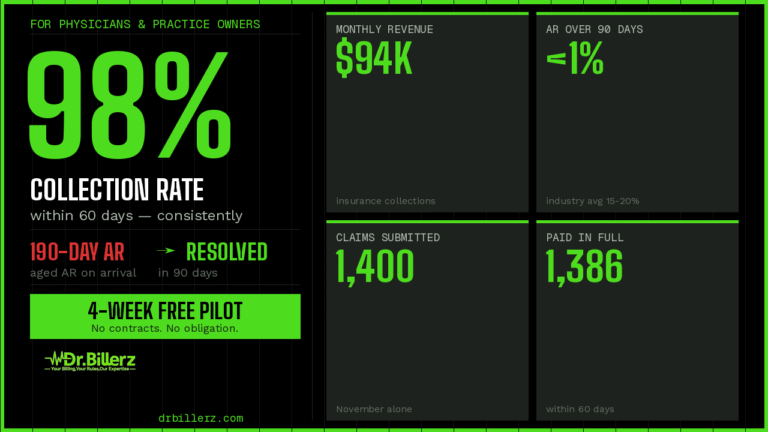
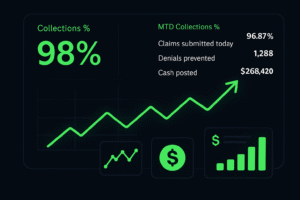
98% collection rate — across the entire practice.
$94,000 in insurance revenue per month, consistently.
In November alone: 1,400 claims submitted. 1,386 paid in full within 60 days. Less than 1% aging past 90 days.
That’s not a strong month. That’s what the baseline looks like when the system is working correctly.
The Pattern We See Again and Again
Practices that come to us with aging AR almost never have a biller problem. They have a process problem. The billers are busy. The claims are going out. But without a forensic layer — without someone actually diagnosing why denials recur, why AR ages, why cash flow is inconsistent — the activity never translates into results.
Busy billing is not the same as effective billing.
The standard we hold every Dr. Billerz engagement to: 98%+ of monthly revenue collected within 60 days. Less than 1% of insurance AR over 90 days. Not as a target — as a process outcome.
What This Means for Your Practice
If your AR is aging and you’re not sure why, the answer is almost always in the audit — not the claims. The claims are the symptom. The audit finds the disease.
We offer a 4-week free pilot for practices that want to see what this looks like in their own revenue cycle. No contracts. No obligation. You see the numbers before you make any decision.
If your collections are below where they should be — or if you’ve simply stopped knowing what “where they should be” even looks like — that’s the conversation worth having.
Book a free 15-minute call at drbillerz.com, or email info@drbillerz.com.
Your billing shouldn’t be a guessing game. And your AR shouldn’t be telling you stories you don’t understand.